I recently hosted a webinar on Medicare updates in 2018 with compliance expert, Nancy Beckley, discussing what therapists need to know for compliance success in the New Year (view the recording here). We received many questions ranging from the Medicare Therapy Cap and Fee Schedule to evaluation codes and specific sections of the ACA.
In this blog, you’ll find an overview of the themes we were most asked about. Don’t see what you’re looking for? Comment below with your question or reach out on Twitter, @HendersonPDX.
Medicare Fee Schedule
We received a lot of questions about the Medicare Fee Schedule for 2018. As we stated in the webinar, reimbursements in the fee schedule for some of the most commonly used codes for active, more evidence-based treatment (ther ex, manual therapy, therapeutic activities) are reduced, while reimbursement for other codes for passive treatment (ultrasound, massage) were increased.
Regardless of the financial incentives, there is no way to compliantly “swap out” one code for another code. The treatment you provide should be accurately reflected by the codes on the claim form. For example, substituting the massage code for the manual therapy code when the treatment provided is more accurately described by the manual therapy code is fraudulent. When in doubt, look at the description of the CPT code.
For any questions regarding specific changes in the fee schedule, consult your Medicare Contractor’s website.
Also, please keep in mind that the example utilized in the webinar did not take into account multiple procedure payment reduction or sequestration adjustments. Taking those into account, there may be up to a 5% decrease in reimbursement for visits that utilize the commonly used codes.
Lastly, there was a typographical error on slide 24. One of the column headers was labeled “Fee per Visit” instead of “Fee per Unit”. We apologize for the error.
Medicare Cap
Repeal or Not?
The state of the Medicare Cap is in flux for 2018 and confusion reigns. There were efforts to repeal the cap at the end of 2017, but at this time the cap is still in place AND the exceptions process for 2018 has not been extended.
Here’s an overview of the possibilities we faced. As I’m sure you know by now, we ended up with option 4.
- Cap is Repealed: It seems doubtful that Congress will get this done, but if the cap is repealed, there will still be a requirement to apply the KX at $3,000. Applying the KX indicates that Medicare may elect to manually review for medical necessity. (In essence, from our client’s perspective, there is no real change except the KX is applied a little later.)
- Cap is Not Repealed, Exceptions Process is Not Reinstated: If that is the case, there will be a “hard cap” at $2010 and Medicare will not pay for services beyond that amount. To bill the patient for services beyond the cap, our clients would need to collect an ABN. Based upon the MACRA legislation, if this scenario happens, hospitals outpatient therapy for provider-based clinics will NOT be subject to the therapy cap.
- Cap is Not Repealed, Exceptions Process is Reinstated: No changes necessary except adjusting the cap amount to $2010 for 2018. KX would be applied at $2010 for medically necessary services.
- No Action Prior to the End of the Year: We believe that this is the most likely scenario. Congress will not do anything until after the start of the year. With no congressional action, the cap of $2010 will be automatically instated without the exceptions process. Using history as a guide, the exceptions process may be reinstated sometime later, possibly as late as March of 2018. As noted above, per MACRA legislation, hospital outpatient therapy departments will NOT be subject to the therapy cap.
Advanced Beneficiary Notice Misconceptions
In addition to presentations, we have written about ABNs many times in the past, but there are still a lot of misconceptions about the use of the ABN in relation to the Therapy Cap.
In reality, the use of an ABN has nothing to do with the cap. It should only be used to notify the patient that the services you provide are likely not going to be paid by Medicare. If you are providing medically necessary services, you should not ask the patient to sign an ABN, because those medically necessary services are a Medicare benefit.
If you can no longer justify continued treatment on the basis of medical necessity, you should normally discharge the patient. If the patient would like to continue treatment that does not fit the medical necessity criteria, you may continue treating the patient if you notify the patient with an ABN that continued treatment is not necessary and will not be covered by Medicare.
Exceptions Process
Effective January 1, the automatic exceptions process is not in effect. For dates of service prior to January 1, all medically necessary therapy services qualified for an exception to the Medicare Cap automatically. There is no longer a list of diagnosis codes that qualify a patient for an exception.
Quality Payment Program
We briefly discussed MIPS and the Quality Payment Program. At this writing, we do not know if PT, OT and Speech will become eligible professionals for MIPS participation in 2019. But, in the meantime, we urge you to become familiar with the components of the program. The CMS website is the best place to start: https://qpp.cms.gov/.
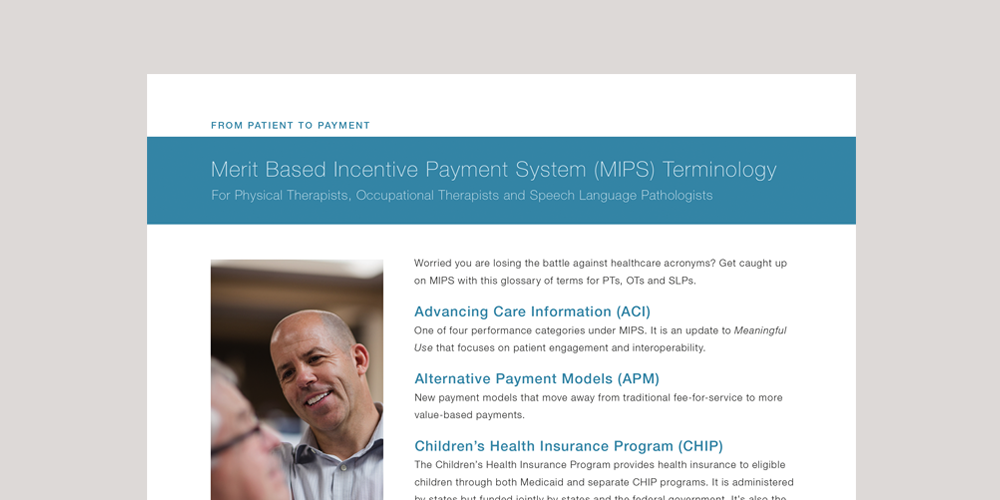
Feeling lost in a fog of MIPS terminology? Download our MIPS glossary to gain a better understanding of its common and not so common terms.
Download GlossaryWe also recommend continued reporting of Quality Measures (formerly PQRS), which is an important component of MIPS. We will provide more details on successfully participating in MIPS in the upcoming year as we learn more.
Evaluation Codes
As Nancy and I discussed, 2018 was a demonstration year for the new complexity based evaluation codes. As Nancy aptly puts it, “we are no longer in the sandbox.” While there is still no differential payment from Medicare, there is some from other payers.
We provided a number of resources on the selection of appropriate evaluation codes last year. We recommend reviewing those resources and training your staff.
- Decision Matrix for Evaluation Codes
- OT Eval Codes
- Webinar Recording July 2016: Includes information on preparing for the new evaluation codes.
Other Thoughts
In the “everything else” category, we received questions during the webinar, as well as follow-up questions, specifically related to Nancy’s comments on Section 1557 of the Affordable Care Act. In our follow up webinar on January 23rd, Nancy will take a few minutes to give the legal mandate for Section 1557 compliance and why private practices who accept Medicaid and TRICARE are subject to Section 1557 (look for this registration to come soon). Hospitals, rehab agencies, CORFs, SNFs and Home Health Agencies are subject to the law as Part A Medicare Providers, however private practice compliance with the law is triggered in other elements.
Maintenance therapy is a benefit and is not affected by the therapy cap or the need for the KX modifier. The KX modifier is only applicable when the exceptions process is in place, or other legislation indicates the use of the modifier to signify the medical necessity of therapy is supported by documentation. Note: the bipartisan proposed legislation to eliminate the therapy cap requires the appending of the KX modifier to all therapy claims lines over $3000.
There is a lot of concern over payment reform for SNFs for Part A stays. We generally don’t cover that in our webinars designed for Medicare outpatient therapy, and ask our loyal listeners to tune into the constituency groups that are most involved with payment reform in SNFs including NASL and AHCA. Also reach out to APTA, AOTA and ASHA for their analysis on SNF reform.
Looking for more info? Don’t miss my blog from last week all about managing 2018 Medicare cuts.

Comments